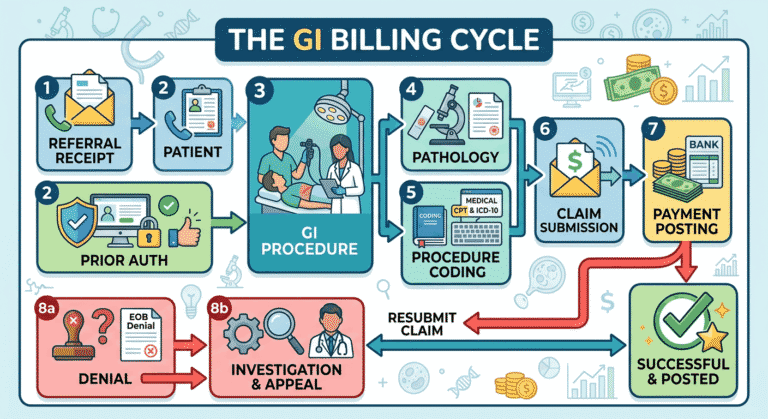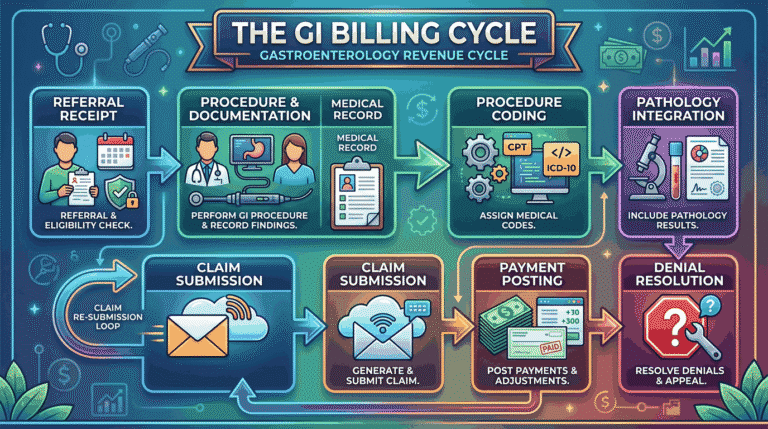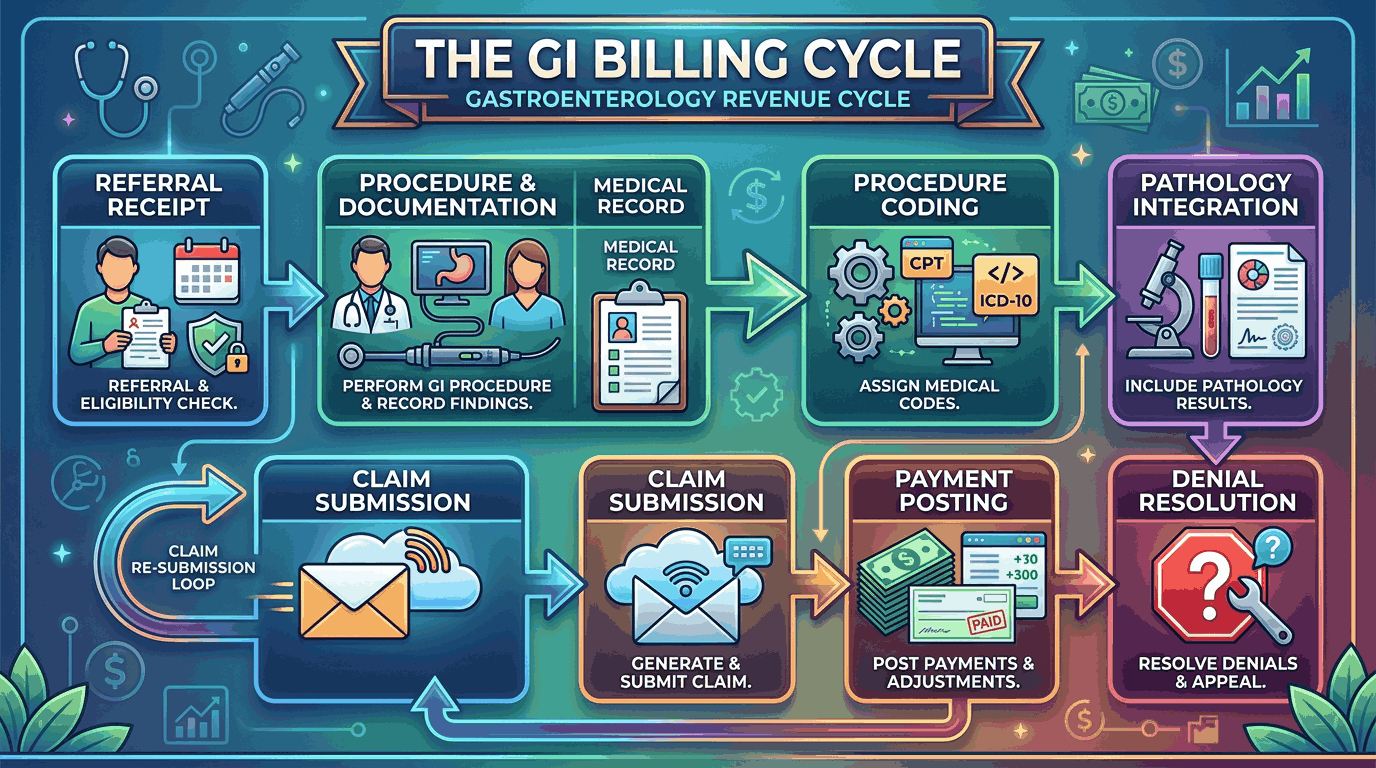
Gastroenterology practices perform some of the most complex and highest-value procedures in outpatient medicine. Yet GI groups consistently rank among the hardest-hit specialties for claim denials and underpayments. The reason is clear: endoscopic coding, screening-versus-diagnostic designation rules, and multi-procedure bundling create a billing minefield that general teams cannot navigate.
Specialized gastroenterology billing services solve this problem at the root. When certified GI coders manage your revenue cycle, every colonoscopy, every biopsy, and every add-on polypectomy generates the full reimbursement your practice deserves.
This guide explains exactly how gastroenterology medical billing services work, where GI practices lose the most revenue, and how to choose a billing partner that permanently closes those gaps.
What Are Gastroenterology Billing Services?
Gastroenterology billing services manage the specialized revenue cycle for GI practices, endoscopy centers, and ambulatory surgery centers performing digestive system procedures. These services include insurance verification, pre-procedure authorization, endoscopic procedure coding, pathology charge coordination, multi-code claim submission, payment reconciliation, denial management, and patient collections. Because gastroenterology involves high-value procedures with intricate coding rules, dedicated billing expertise directly determines whether a GI practice thrives financially or bleeds revenue through preventable errors.
Why Gastroenterology Billing Demands Specialty Expertise
No two medical specialties bill identically, but gastroenterology presents a unique combination of challenges that make generic billing approaches exceptionally dangerous.
Screening vs. Diagnostic Colonoscopy Designation
This single distinction drives more GI billing errors and more patient complaints than any other factor. A screening colonoscopy (CPT 45378) for an average-risk patient carries specific payer coverage rules under the Affordable Care Act. When a polyp is discovered and removed during a screening procedure, the claim must convert to a diagnostic/therapeutic colonoscopy with the appropriate polypectomy code.
Here is where the complexity explodes. Some payers cover the converted procedure at 100% as preventive care. Others apply deductibles and coinsurance once the procedure becomes diagnostic. Incorrect claim designation triggers patient billing errors, payer disputes, and compliance risk simultaneously.
A dedicated gastroenterology billing team tracks payer-specific rules for screening conversion and applies the correct coding, modifiers, and diagnosis codes to protect both revenue and patient trust.
Endoscopic Procedure Coding Complexity
GI endoscopy involves a dense web of CPT codes, each describing a specific technique, anatomical location, and intervention level:
45378: Diagnostic colonoscopy
45380: Colonoscopy with biopsy
45385: Colonoscopy with polypectomy by snare
45388: Colonoscopy with ablation of tumor or polyp
43239: Upper GI endoscopy (EGD) with biopsy
43247: EGD with removal of foreign body
43251: EGD with removal of tumor or polyp by snare
When a gastroenterologist performs multiple interventions during a single endoscopic session a biopsy in the ascending colon, a snare polypectomy in the sigmoid, and a hot biopsy in the transverse each intervention may qualify for separate billing with the correct modifier. Missing any of these distinct services surrenders revenue the physician has already earned.
Expert gastroenterology medical billing services review every operative and pathology report to capture the complete scope of work.
Multi-Procedure Reduction Rules
When multiple endoscopic procedures occur during the same session, payers apply multi-procedure payment reduction (MPPR) rules. The highest-valued procedure receives full payment. Subsequent procedures receive reduced reimbursement typically 50% of the allowed amount under Medicare rules.
Understanding which procedure to list as the primary code and sequencing additional procedures correctly maximizes total reimbursement. A common billing mistake lists the lower-value procedure first, causing the higher-value service to receive the reduced payment. This sequencing error alone can cost $200 to $500 per case.
A skilled GI billing partner sequences every claim strategically to ensure the highest possible total payment.
Core Components of Top-Tier Gastroenterology Billing Services
Comprehensive GI billing covers every stage of the revenue cycle with specialty-specific precision:
Pre-Procedure Authorization: Verifying insurance coverage, confirming procedure-specific prior authorization, and documenting medical necessity before the patient arrives for their endoscopy.
Certified GI Coding: Coders trained specifically in gastroenterology CPT codes, ICD-10 digestive system diagnoses, and HCPCS supply codes assign accurate codes for every procedure, biopsy, and intervention.
Pathology Charge Coordination: Synchronizing endoscopy procedure codes with corresponding pathology specimen codes to ensure complete billing for both the procedural and laboratory components of each case.
Modifier Mastery: Correct application of modifiers 59 (Distinct Procedural Service), XE/XS/XP/XU (Separate Encounter/Structure/Practitioner/Unusual Non-Overlapping), 26 (Professional Component), 52 (Reduced Services), and 53 (Discontinued Procedure).
Clean Claim Submission: Every claim scrubbed against NCCI bundling edits, LCD medical necessity criteria, and payer-specific processing rules before electronic filing.
Payment Posting and Underpayment Detection: Systematic comparison of every ERA/EOB against contracted fee schedules to identify and recover payer shortfalls.
Denial Management and Appeals: Root-cause investigation of every rejection, with rapid corrective resubmission and clinical documentation-supported appeals.
ASC and Office-Based Billing: Managing the distinct billing rules for procedures performed in ambulatory surgery centers versus office-based endoscopy suites.
Revenue-Destroying GI Billing Errors to Eliminate
These common mistakes silently drain gastroenterology practice revenue:
Failing to Bill Polyp Removal Separately: When a screening colonoscopy converts to a therapeutic procedure with polypectomy, both the colonoscopy and the polypectomy technique must appear on the claim with correct modifiers. Submitting only the base colonoscopy code forfeits the polypectomy reimbursement entirely.
Missing Biopsy Charges: Pathology specimens taken during endoscopy require separate CPT codes. If the operative report documents four biopsies from distinct sites, each qualifies for individual billing. Generic billers often submit a single biopsy code regardless of specimen count.
Incorrect Diagnosis Code Pairing: Payers deny GI claims when the submitted ICD-10 diagnosis does not support medical necessity for the procedure. Coding a screening colonoscopy with a symptom-based diagnosis or vice versa triggers immediate rejection.
Ignoring Moderate Sedation Changes: CMS removed moderate sedation from many endoscopy codes in recent years, requiring separate billing for sedation services when applicable. Practices unaware of this change lose sedation reimbursement on every qualifying case.
Overlooking Infusion Therapy Billing: GI practices administering biologic infusions (Remicade, Entyvio, Stelara) in-office must accurately bill the drug cost, administration codes, and associated E/M services. Unbilled or underbilled infusion sessions represent major lost revenue.
In-House Billing vs. Outsourced GI Billing Partner
The In-House Burden
Gastroenterology coding requires specialized training that most general medical billers lack. Recruiting coders with genuine GI endoscopy experience means competing for a small talent pool at premium salaries. Add software costs, clearinghouse fees, continuing education, and benefits, and the fixed overhead strains practice margins.
When your lead GI coder leaves, the impact is immediate. Endoscopy claims require too much specialty knowledge for a temp or cross-trained employee to handle accurately. Backlogs build. Denials spike. Revenue stalls.
The Outsourcing Edge
A gastroenterology billing partner maintains a dedicated team of GI-certified coders and billing specialists. Volume fluctuations whether from seasonal screening pushes or provider schedule changes are absorbed seamlessly. The company invests in endoscopy-specific coding tools, payer intelligence databases, and continuous training that no single practice can cost-justify independently.
Performance-based pricing ties the billing company’s revenue directly to your collections, ensuring permanent alignment of financial incentives.
KPIs for Gastroenterology Revenue Cycle Excellence
Demand visibility into these metrics from any billing partner:
Clean Claim Rate: Percentage of claims paid on first submission. Target 96% or higher for GI-specific claims.
Average Revenue Per Procedure: Total collections divided by total endoscopic procedures. This metric reveals whether charge capture and code sequencing maximize case value.
Days in Accounts Receivable: Average time between procedure date and payment receipt. Maintain below 32 days for optimal GI practice cash flow.
Denial Rate: Percentage of rejected claims. A strong gastroenterology billing partner keeps this below 3.5%.
Net Collection Rate: Total collected versus total allowable charges. Elite GI billing teams exceed 98%.
Pathology Charge Capture Rate: Percentage of endoscopic cases with corresponding pathology billing. Anything below 95% signals missed specimen charges.
How to Choose the Right Gastroenterology Billing Partner
Follow this evaluation process to identify a partner equipped for GI-specific complexity:
Verify Endoscopy Billing Experience: Ask specifically about colonoscopy, EGD, ERCP, and capsule endoscopy billing volume. Reject companies whose GI experience is limited to office-based E/M coding.
Assess Screening Conversion Expertise: Present a scenario: a screening colonoscopy converts to diagnostic with snare polypectomy. Ask the vendor to walk through their coding, modifier, and diagnosis code approach. Their answer reveals whether they truly understand GI billing.
Evaluate Pathology Coordination: Confirm the billing team cross-references operative reports with pathology results to ensure complete specimen-level billing. This coordination step separates expert GI billing from generic claim submission.
Demand Real-Time Reporting: Accept nothing less than dashboard access showing per-procedure revenue, denial trends by code, payer performance comparisons, and provider-level productivity metrics.
Confirm ASC and Office Billing Capability: If your practice operates both an office endoscopy suite and an ambulatory surgery center, the billing company must manage both facility types under their distinct payment models.
Review Compliance Protocols: Verify regular internal coding audits, HIPAA compliance documentation, and adherence to OIG guidelines for GI-specific risk areas.
The Infusion Therapy Revenue Opportunity
GI practices increasingly administer biologic infusion therapies for Crohn’s disease, ulcerative colitis, and other inflammatory conditions. These in-office infusion sessions generate substantial revenue, often $2,000 to $10,000 per session when billed correctly.
Accurate infusion billing requires:
Drug codes (J-codes): Precise HCPCS Level II codes for the specific biologic administered, billed per unit based on dosage.
Administration codes: Initial infusion (96413), sequential infusion (96415), and concurrent infusion codes based on timing and technique.
Associated E/M services: When a physician evaluation occurs on the same day, modifier 25 separates the E/M from the infusion service.
Pre-authorization: Most biologics require prior authorization. Missing or expired authorizations result in full claim denial.
Gastroenterology medical billing services that capture infusion revenue accurately can add six figures annually to a GI practice’s bottom line.
Frequently Asked Questions
What are gastroenterology billing services?
Gastroenterology billing services manage the complete revenue cycle for GI practices and endoscopy centers. They handle procedure-specific coding for colonoscopies, EGDs, and other endoscopic interventions, along with pathology coordination, claim submission, denial management, and patient collections tailored to digestive health specialties.
Why do GI practices have high denial rates?
Gastroenterology claims face frequent denials due to screening-versus-diagnostic designation errors, incorrect procedure sequencing, missing medical necessity documentation, improper modifier use on multi-procedure cases, and failure to coordinate endoscopy codes with pathology specimen billing.
How much do gastroenterology billing services cost?
Most GI billing companies charge between 4% and 8% of net collections. Rates vary based on procedure volume, payer mix, number of providers, and whether ASC facility billing is included. Performance-based pricing ensures the billing company earns revenue only when your practice collects successfully.
How quickly can a GI billing company improve my revenue?
Practices typically see measurable results within 45 to 75 days. Denial rates decrease, per-procedure revenue increases, and AR days shorten as the new team implements specialty-specific coding protocols and aggressive payer follow-up.
Can a billing company handle both my office and ASC billing?
Yes. Experienced gastroenterology billing services manage professional fee billing for physicians alongside facility billing for ambulatory surgery centers. They understand the distinct fee schedules, payment methodologies, and claim formats required for each setting.
Collect the Full Value of Every Procedure
Your gastroenterologists perform technically demanding procedures that improve and save lives. Every colonoscopy, every polypectomy, every infusion session represents clinical expertise that deserves complete financial recognition.
Generic billing teams cannot protect GI revenue. The coding is too complex. The payer rules shift too frequently. The margin for error is too thin. Only a partner with deep endoscopy coding knowledge, pathology coordination discipline, and relentless payer follow-up can ensure your practice collects every dollar it earns.
Ready to maximize your GI practice revenue? Discover how an experienced gastroenterology billing partner can eliminate denials, capture every procedure code, and accelerate your collections starting today.